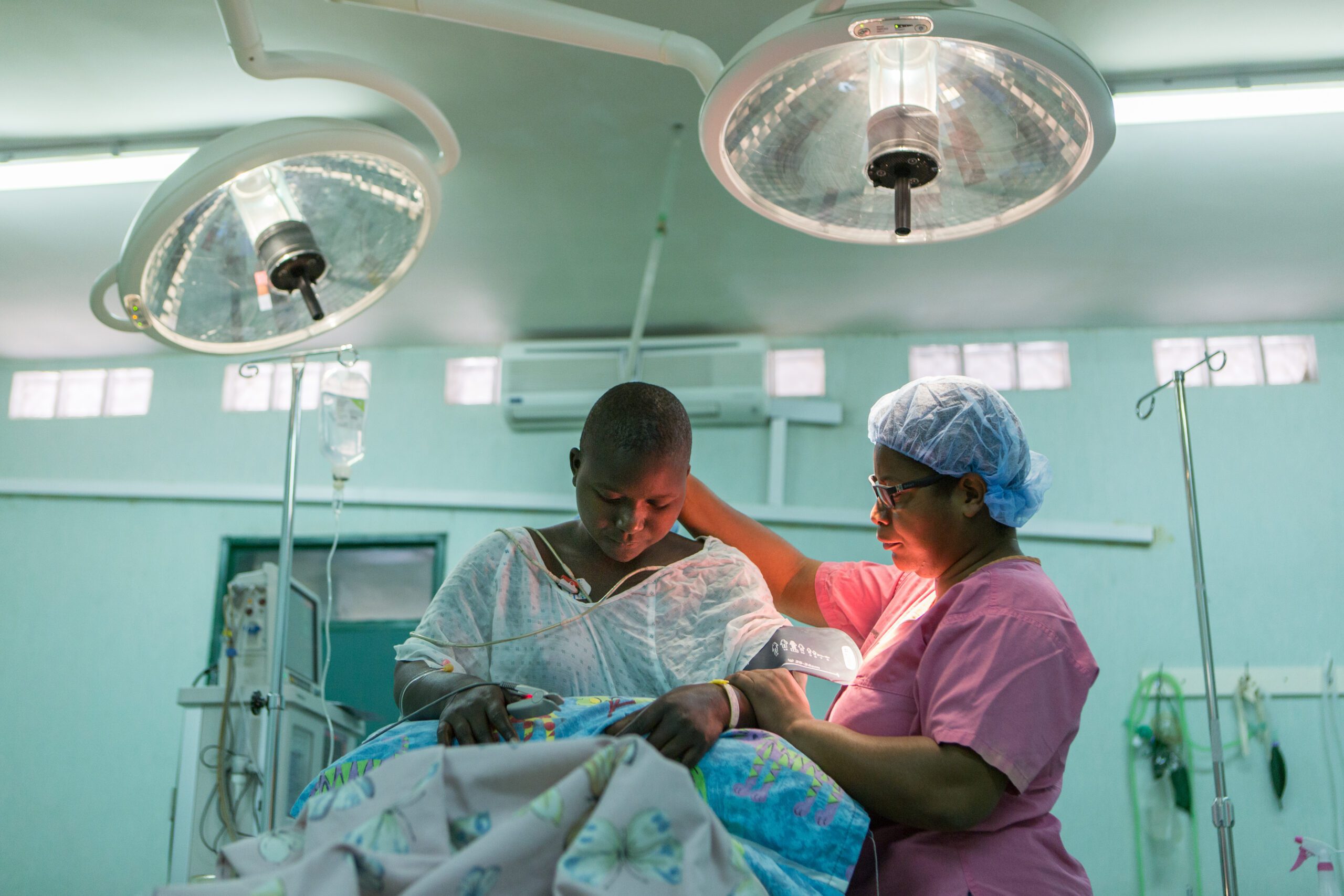
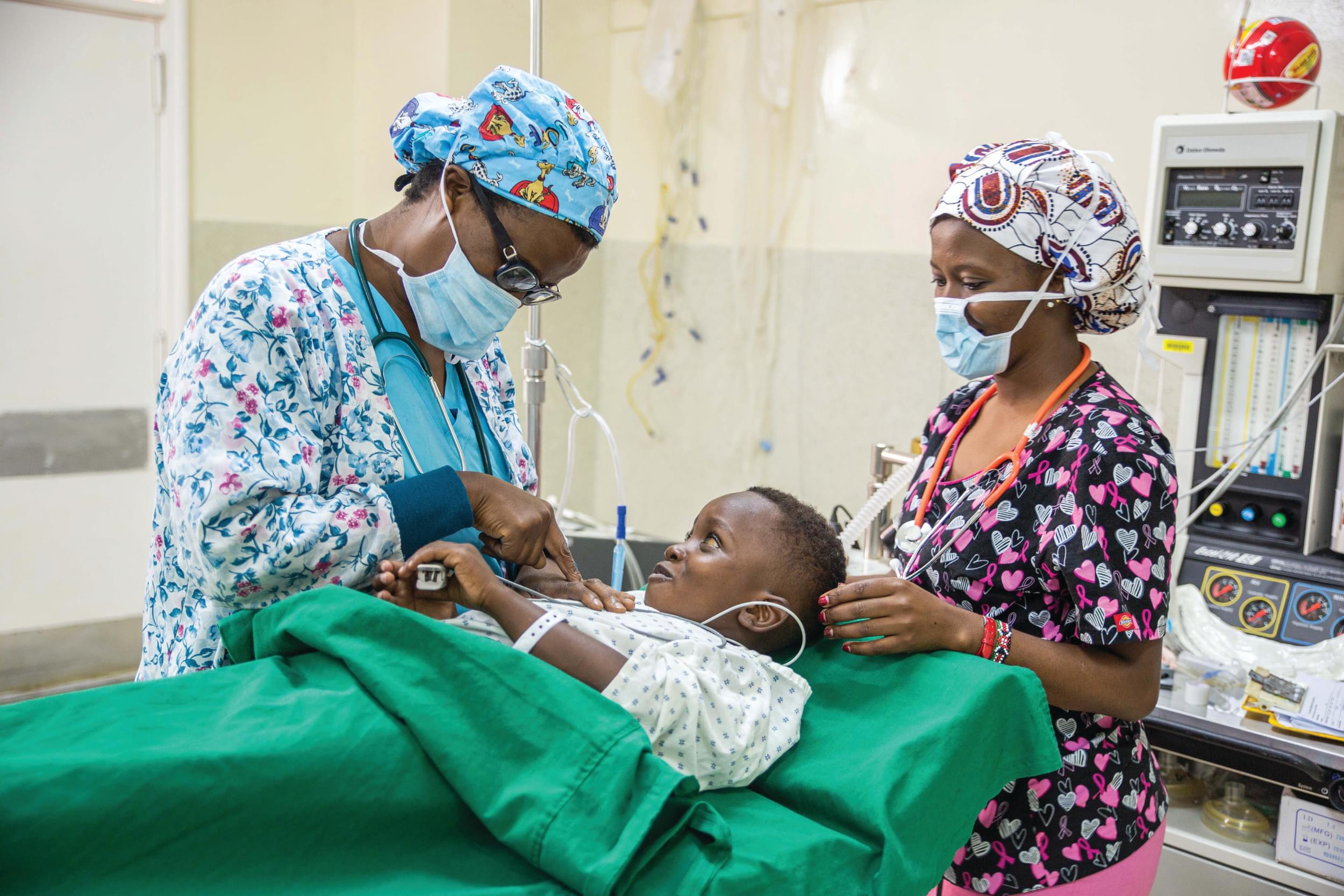
In the past two decades much emphasis was placed on primary healthcare, including prevention and management of infectious diseases, as well as mother and child care. The millennium development goals had three goals targeting such areas: reduce child mortality, improve maternal health, and combat HIV/AIDS, malaria, and other diseases.
The global health agenda is now changing with a growing realisation that non-communicable diseases play an increasing role in the global burden of disease—even in low- and middle-income countries.
Whilst some non-communicable diseases relate to degenerative disease (such as lifestyle and aging), others may strike younger people and have the potential for curative treatment options. The surgically treatable conditions often fall into this category. Injury is one such bracket of disease which kills more people than all the communicable diseases combined. Of those who die from injury, 90% live in low- and middle-income countries, and the majority are young males. For every one who dies, at least 10 remain with permanent disability. Improved emergency surgical care systems could alleviate much of this disease burden.
Whilst “injury”’ is getting some publicity as the most neglected global disease entity (albeit still not specifically mentioned in the sustainable development goals), elective surgical interventions for children with physical deformities and disabilities also suffer from a lack of awareness.
It may seem expensive to provide elective surgical care for children, but these individuals expect to have many remaining years of life, and a one-off intervention may achieve a transformative increase in their life potential. In this way, the cost per DALY (disability adjusted life year) may be significantly cheaper than more established medical treatments for cancer, cardiac disease, or even HIV.

Several particular areas of surgical care for children offer great economic value and are supported by high quality evidence. These should be considered as “Essential Children’s Surgical Procedures,” and include inguinal hernia repair, trichiasis surgery, cleft lip and palate repair, circumcision, congenital heart surgery, and orthopedic procedures. Our recommendations align with those of a study in the World Journal of Surgery which aimed to draw the link between surgery and public health. It is important to prioritize surgical care based on health burden, success of a surgical intervention, and cost-effectiveness. We strongly advocate for increased investment in these “Essential Children’s Surgical Procedures” to improve health for children and gain economic benefit for a society.1
The context for provision of surgical services is a challenge even in high-income countries, since emergency care can transfer pressure and reduce efficiency of elective services. Furthermore, mixing the potentially infective environment of emergency care with an environment of clean elective surgery has drawbacks. Specialist elective facilities have potential advantages in quality and efficiency. CURE International is one group supporting specialty elective hospitals for pediatric surgical care in low-income countries. Its hospitals focus on pediatric orthopedic, plastic, and neurosurgical disciplines. Such facilities can be highly effective components of a health service in providing surgical care, with the added ability to deliver high quality training to healthcare workers.2
Another challenge in provision of universal health coverage is the tendency for single disease entities to be promoted and funds to be channeled accordingly. This may happen in communicable disease (eg. malaria) or non-communicable diseases (eg. clubfoot). The advantage of this approach is that it has appeal to donors and celebrity champions. Skills may be developed and measurable gains documented. The disadvantage is that development of health systems which deal with emergency and elective care scenarios would provide a more strategic approach to cover the spectrum of surgically treatable diseases. The facility and skill set to provide cleft lip and palate surgery generally relates closely to that which provides for a wide variety of surgically treatable pediatric conditions. Equally, the facility and skill set which offers laparotomy for acute intestinal obstruction may easily be developed to provide emergency caesarean section and open fracture management. Surgical care systems need to develop in a strategic and coordinated way and not piecemeal, as may happen when driven by external donors who hold specific, focused aims.
Finally, surgical care has reached the global health agenda! As the policy makers advocate for expansion of global surgical access and national surgical plans, clear thinking will be required to plan emergency surgical systems and elective surgical systems and facilities which promote economic and quality services with access for all.
- Saxton AT et al Economic analysis of children’s surgical care in low and middle income countries: systematic review and analysis. PLOS Open access 2016;11(10)e0165480.
- Gocken E. Orthopaedic surgery residency training in East Africa. J Am Acad Orth Surg 2019; 3(7):1-7.
About CURE International
CURE International is a Christian nonprofit organization that operates a global network of pediatric surgical hospitals, which serve one of the world’s most marginalized and vulnerable populations – children with disabilities. Patients at CURE hospitals suffer from orthopedic, neurosurgical, and maxillofacial conditions that limit their mobility/functionality and opportunities for education and employment. In addition to world-class clinical service, CURE intentionally ministers to the emotional and spiritual needs of patients in its care and invests in training programs that aim to equip the next generation of health workers and strengthen national health care systems. Since inception, CURE has conducted more than 5.3 million patient visits and 330,000 surgical procedures around the world. For more information, visit https://cure.org/.