Together we dream of a world without clubfoot where kids can walk.
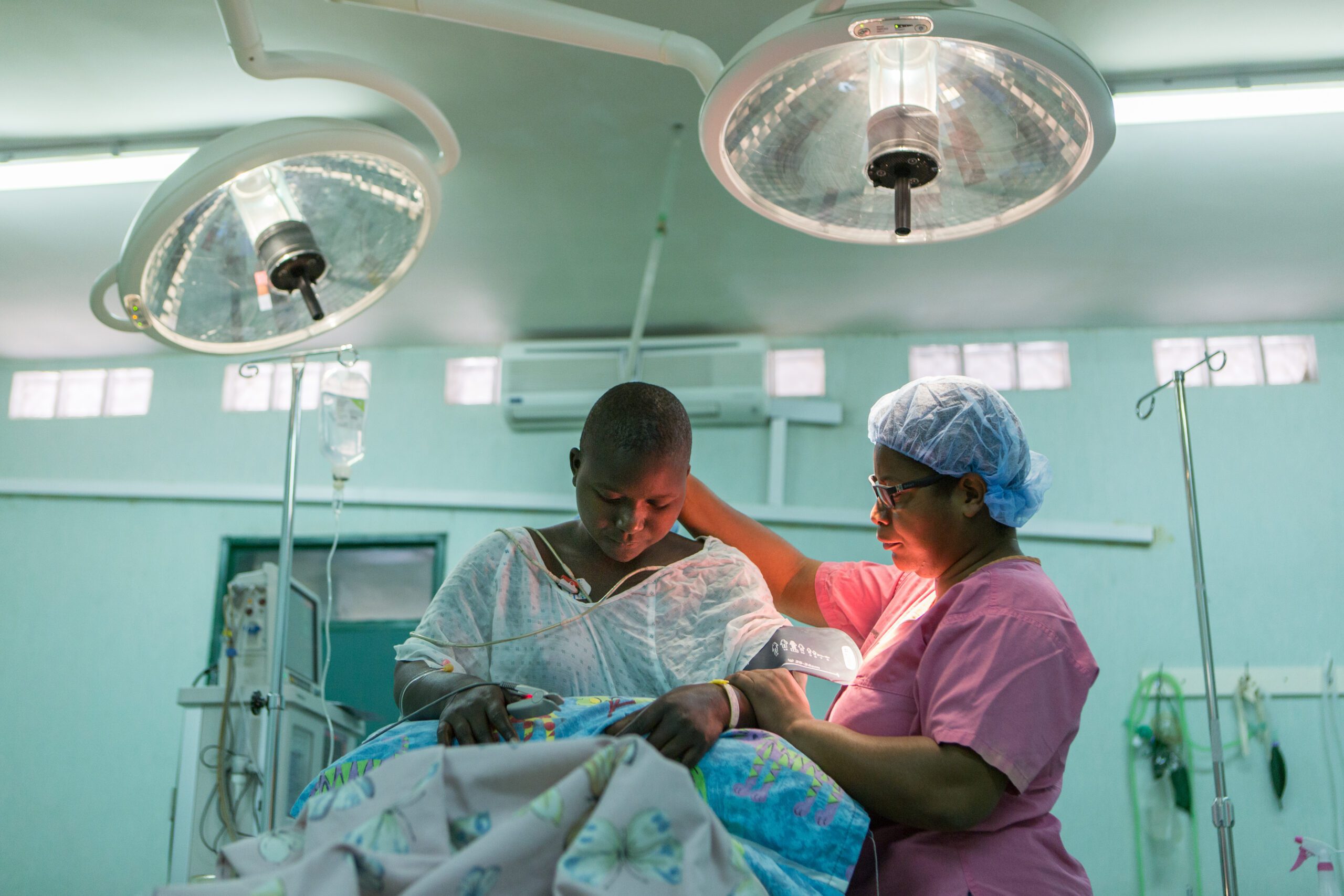
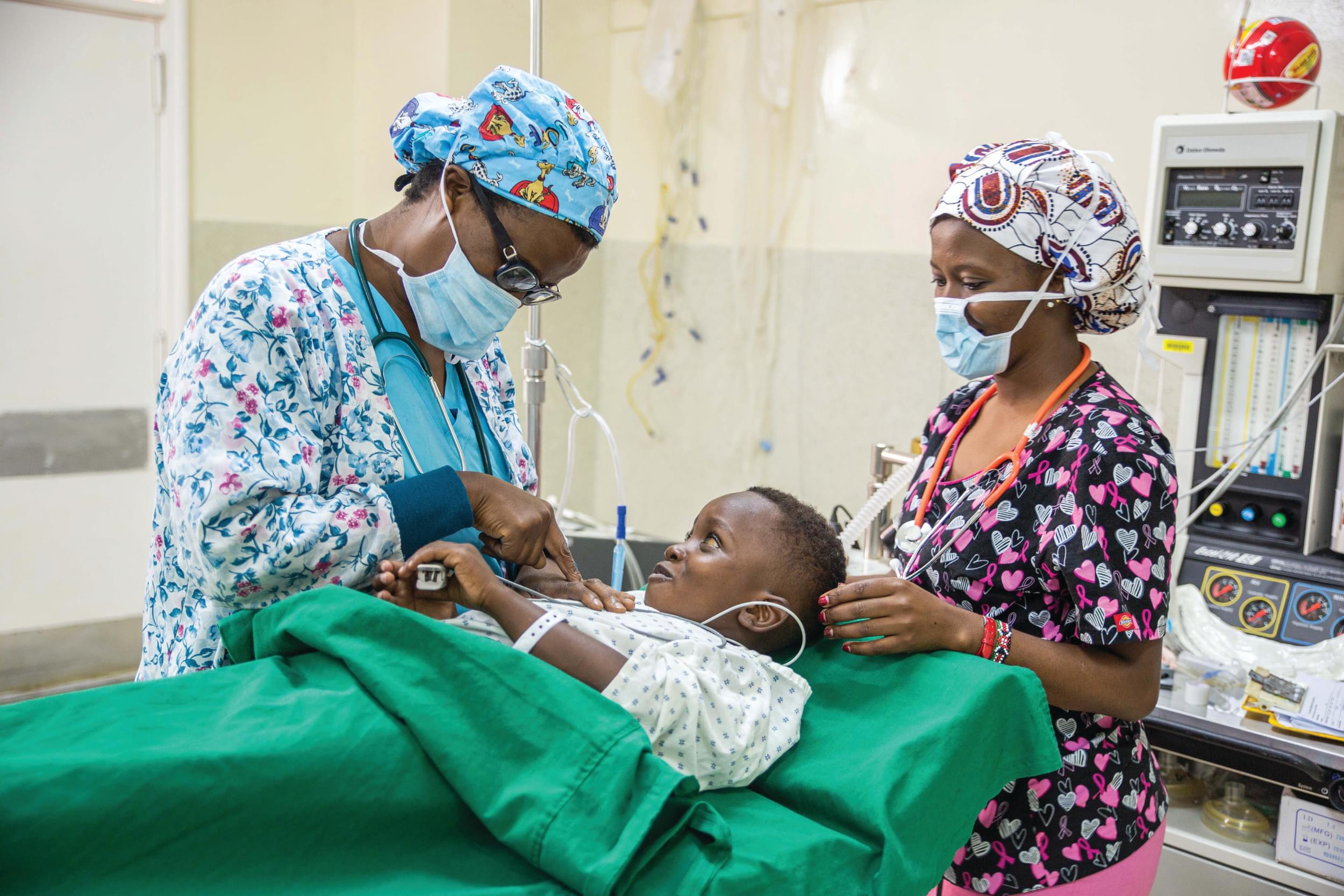
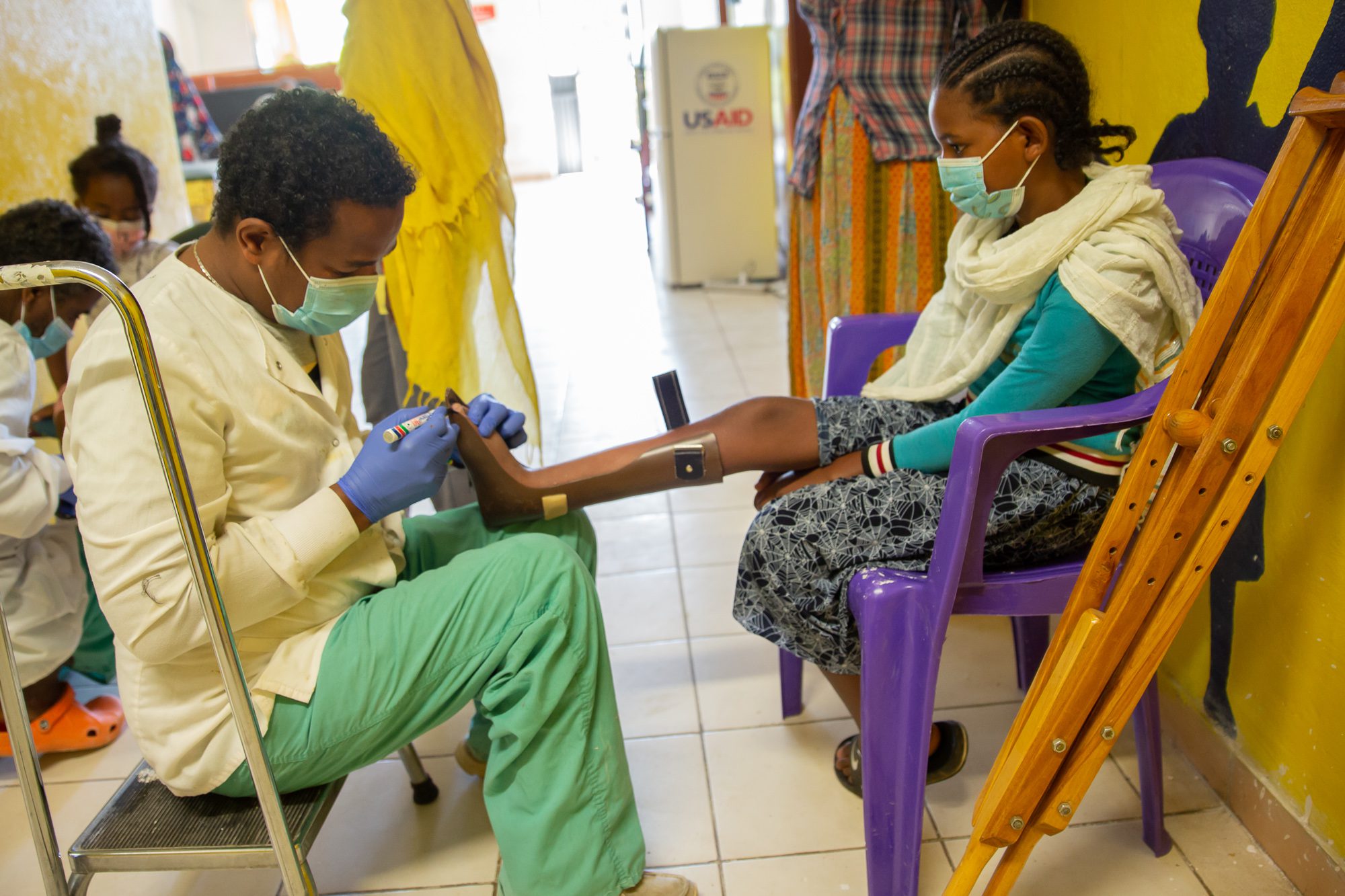
Worldwide, clubfoot is a big problem. In Ethiopia alone, there are an estimated 40,000 children with clubfoot and more being born every year. Clubfoot is a condition where the feet appear to be internally rotated at the ankle. The foot points down and inwards making the sole of the feet face each other, essentially causing the child to walk painfully on the top of their feet. It is a congenital condition that has no known cause. In many of the countries where CURE serves, access to healthcare in rural areas is minimal. The healthcare that is available is often limited and there is no training to treat disabilities such as clubfoot. As a result, many of the children who do seek out treatment are referred to the CURE Children’s Hospital of Ethiopia.
With such a large number of clubfoot patients, CURE Ethiopia along with NDORMS from Oxford University’s Medical Services Division has conducted research and produced studies to develop evidence-based management of older children (ages 2 – 10 years) with clubfoot. This research has radically changed the way clubfoot is treated at CURE Ethiopia.
CURE Ethiopia’s Medical Director Dr. Tim Nunn explains how older children with clubfoot would traditionally receive extensive orthopedic surgery to correct their condition. While the surgery would straighten out the foot, it “typically leaves limited flexibility and range of motion … there was also a high relapse rate, the majority needing further bony surgery later in childhood,” Dr. Nunn recounts. The high volume of treatment and research indicated that patients perform better when, instead of receiving one majorly invasive operation, they received a series of progressive casts which slowly manipulate the foot into a straighter position followed by several minimally invasive surgeries. In the cases studied, very few had any complications or relapses. These patients were also able to gain a level of flexibility and functionality that would not have been possible with the traditional treatment methods. The casting and limited surgical technique are effective, but it is a longer treatment and requires patience and a commitment to the process.

After an earlier project developing training materials for treating children 0 – 2 years with clubfoot, NDORMS experienced a growing number of requests from trainers across sub-Saharan African for similar materials focusing on treating clubfoot in older children 2 – 10 years. With the excellent results seen at CURE Ethiopia paired with the overall simplicity of the process, NDORMS and CURE Ethiopia began developing a new training course. The training course, titled “Principles of Management of Delayed Presenting Clubfoot,” will empower local health providers to treat basic clubfoot cases. Multiplying the number of treatment providers will expand clubfoot management across Ethiopia, allowing more children to receive desperately needed help. Expanded treatment will also decongest CURE Ethiopia’s waiting list, allowing the highly specialized CURE Ethiopia surgeons to focus on truly complex cases.
The development of this course has been made possible thanks to funding from the Africa Grants Programme, which is managed by the Tropical Health Education Trust and funded by Johnson & Johnson.
The course will be piloted in September 2021 for an audience of Ethiopian physical therapists and surgeons. It will then be revised, finalized, and translated into Amharic. Once complete, the course will be made available to other organizations involved in clubfoot training through the Global Clubfoot Initiative (GCI). While initially in English and Amharic, it is hoped the course will follow in the footsteps of the Africa Clubfoot Training (ACT) Project, which is now in use throughout not only Africa but also Asia, South America, and Europe. The ACT Project is a partnership between NDORMS, CURE, GCI, and Hope Walks.
Principles of Management of Delayed Presenting Clubfoot will escort established medical professionals through the entire treatment process. It starts with the initial evaluation of a new patient, offers guidance for manipulation and casting, demonstrates the series of surgeries required, and illustrates the rehabilitation exercises both during casting and once the casts are removed. The course pairs verbal presentations along with intentionally developed video lessons. Dr. Nunn explains that utilizing the medium of video “allows delivery of good content without changing into operating room scrubs, and the techniques for a learner can be reinforced by repeat viewings.”
The NDORMS project leads are Prof Chris Lavy and Grace Drury who has been integral to every step of this research and course development.
About CURE International
CURE International is a Christian nonprofit organization that operates a global network of pediatric surgical hospitals, which serve one of the world’s most marginalized and vulnerable populations – children with disabilities. Patients at CURE hospitals suffer from orthopedic, neurosurgical, and maxillofacial conditions that limit their mobility/functionality and opportunities for education and employment. In addition to world-class clinical service, CURE intentionally ministers to the emotional and spiritual needs of patients in its care and invests in training programs that aim to equip the next generation of health workers and strengthen national health care systems. Since inception, CURE has conducted more than 5.3 million patient visits and 330,000 surgical procedures around the world. For more information, visit https://cure.org/.