A review of existing trauma and musculoskeletal impairment (TMSI) care capacity in East, Central, and Southern Africa
Abstract:
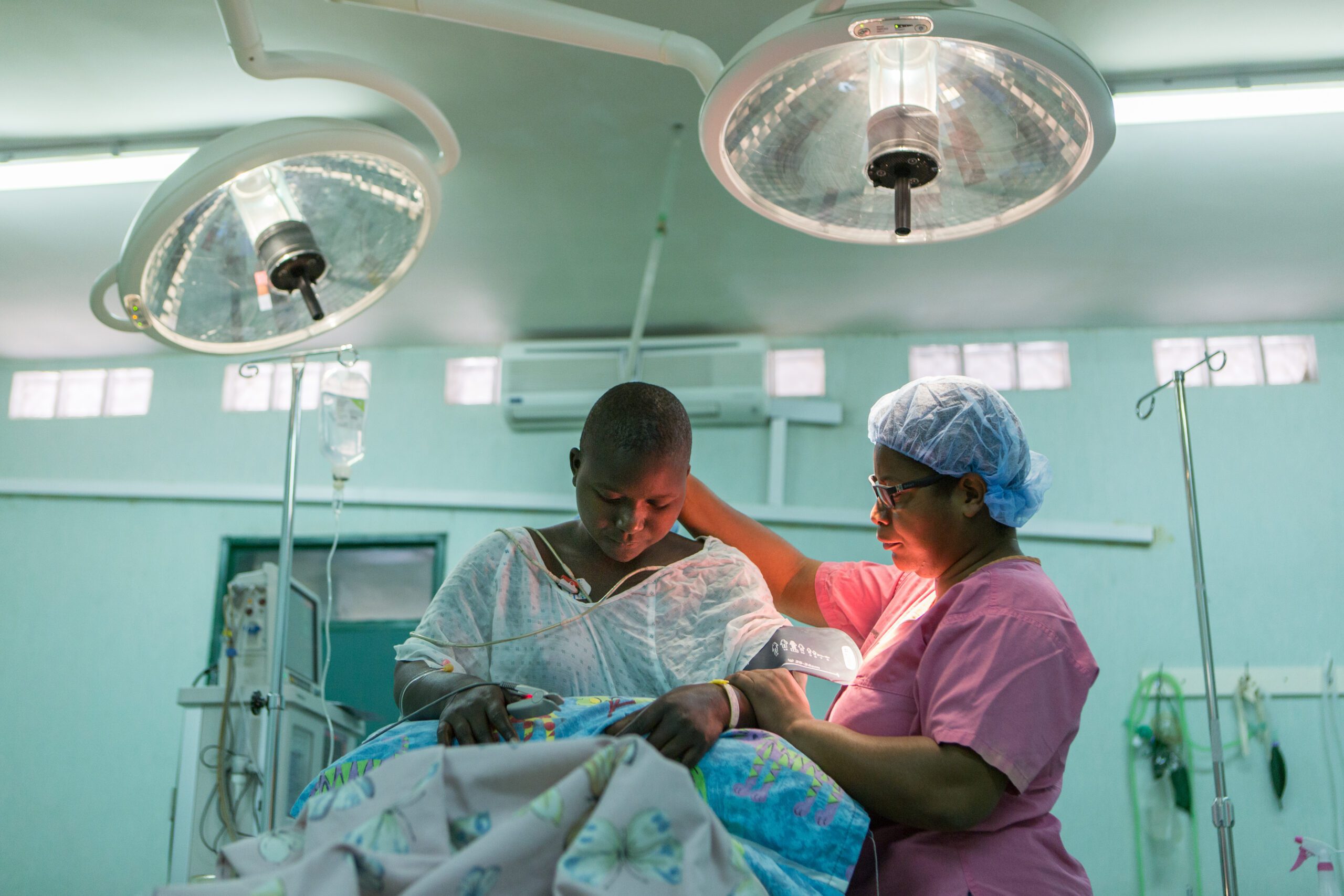
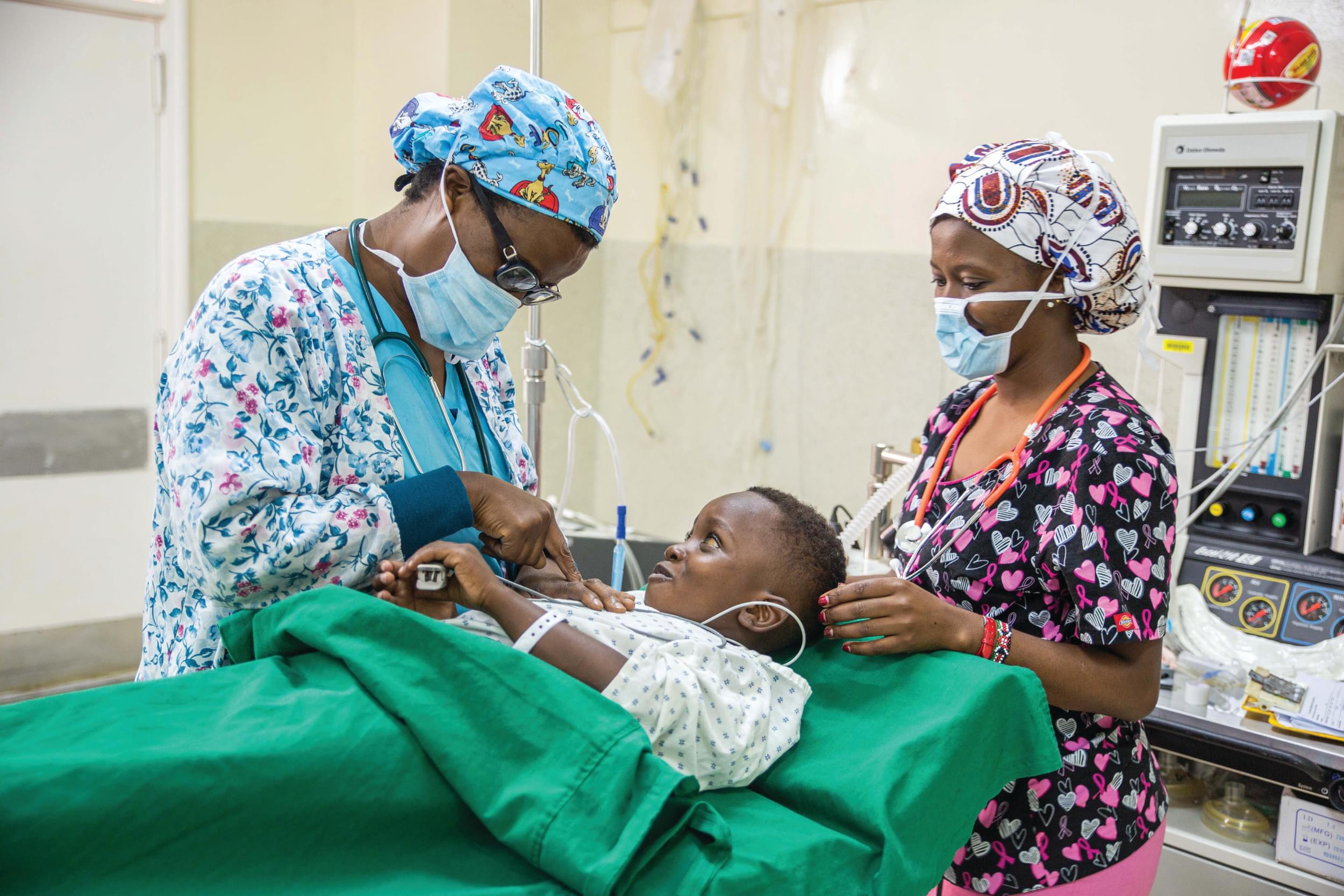
Background: We conducted an assessment of orthopaedic surgical capacity in the following countries in East, Central, and Southern Africa: Burundi, Ethiopia, Kenya, Malawi, Mozambique, Rwanda, Tanzania, Uganda, Zambia, and Zimbabwe.
Methods: We adapted the WHO Tool for Situational Analysis to Assess Emergency and Essential Surgical Care with questions specific to trauma and orthopaedic care. In May 2013–May 2014, surgeons from the College of Surgeons of East, Central and Southern Africa (COSECSA) based at district (secondary) and referral (tertiary) hospitals in the region completed a web-based survey. COSECSA members contacted other eligible hospitals in their country to collect further data.
Findings: Data were collected from 267 out of 992 (27%) hospitals, including 185 district hospitals and 82 referral hospitals. Formal accident and emergency departments were present in 31% of hospitals. Most hospitals had no general or orthopaedic surgeons or medically-qualified anaesthetists on staff. Functioning mobile C-arm X-ray machines were available in only 4% of district and 27% of referral hospitals; CT scanning was available in only 3% and 26%, respectively. Closed fracture treatment was offered in 72% of the hospitals. While 20% of district and 49% of referral hospitals reported adequate instruments for the surgical treatment of fractures, only 4% and 10%, respectively, had a sustainable supply of fracture implants. Elective orthopaedic surgery was offered in 29% and Ponseti treatment of clubfoot was available at 42% of the hospitals.
Interpretation: The current capacity of hospitals in sub-Saharan Africa to manage traumatic injuries and orthopaedic conditions is significantly limited. In light of the growing burden of trauma and musculoskeletal impairment within this region, concerted efforts should be made to improve hospital capacity with equipment, trained personnel, and specialist clinical services.