Costs and benefits of neurosurgical intervention for infant hydrocephalus in sub-Saharan Africa
Abstract:
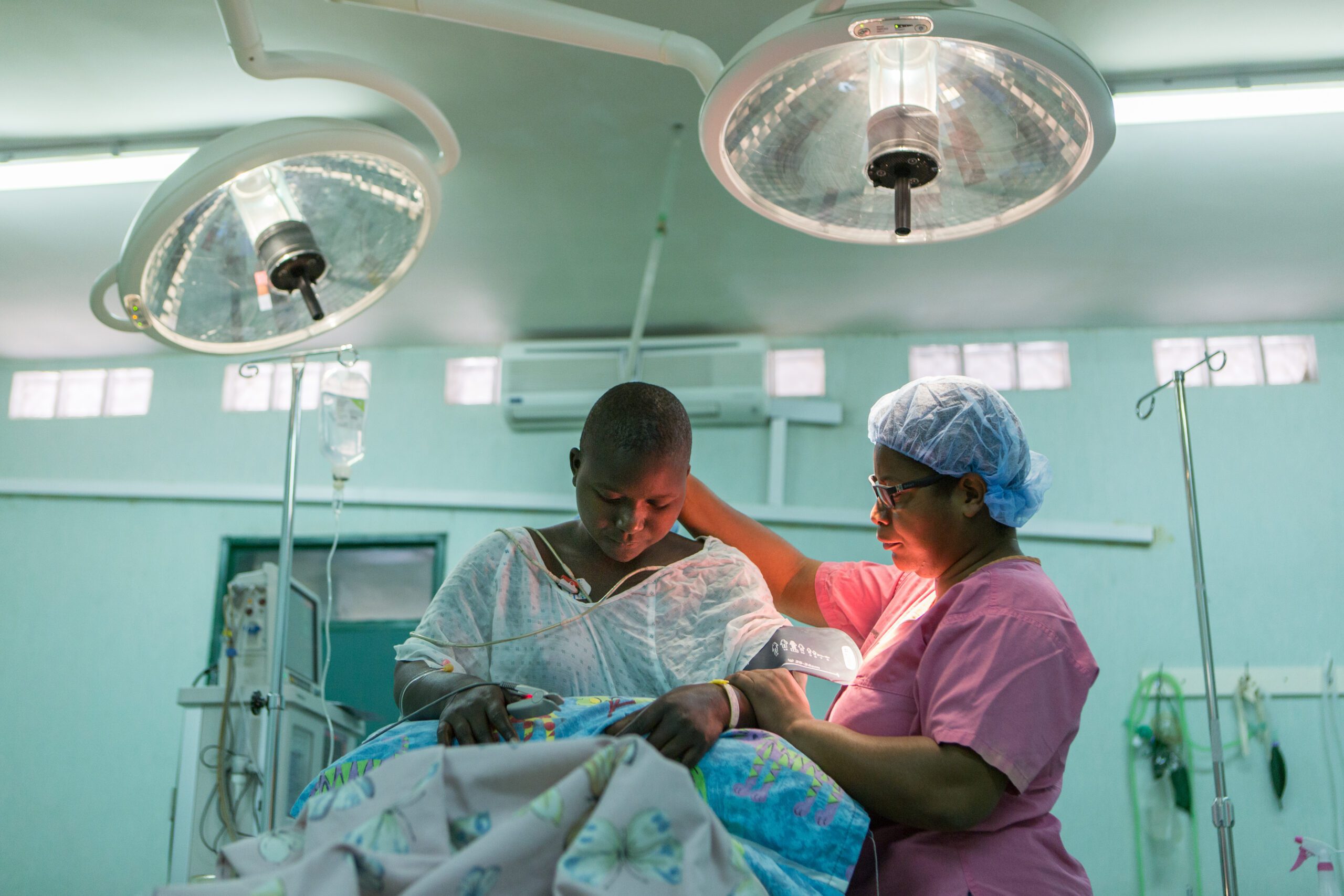
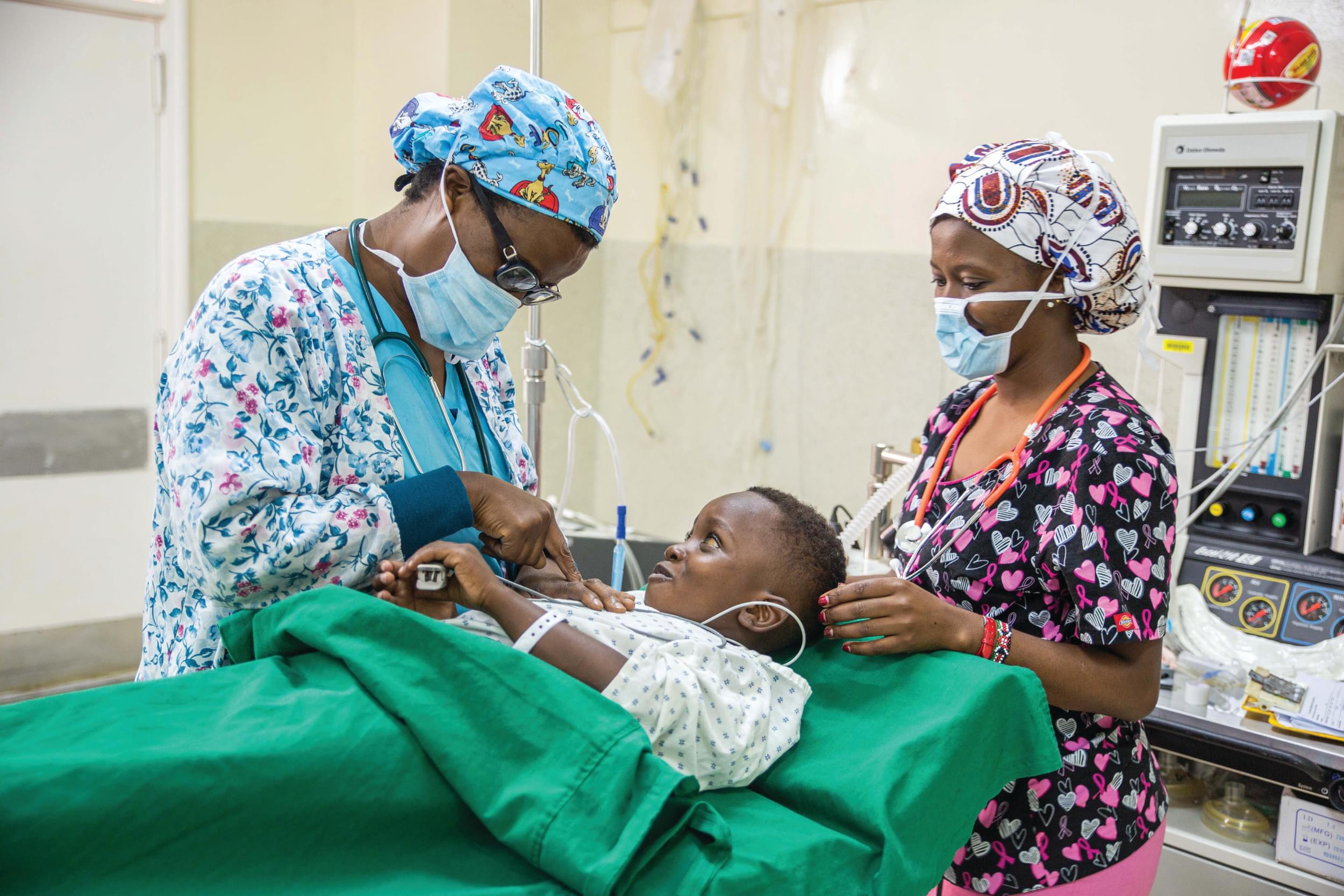
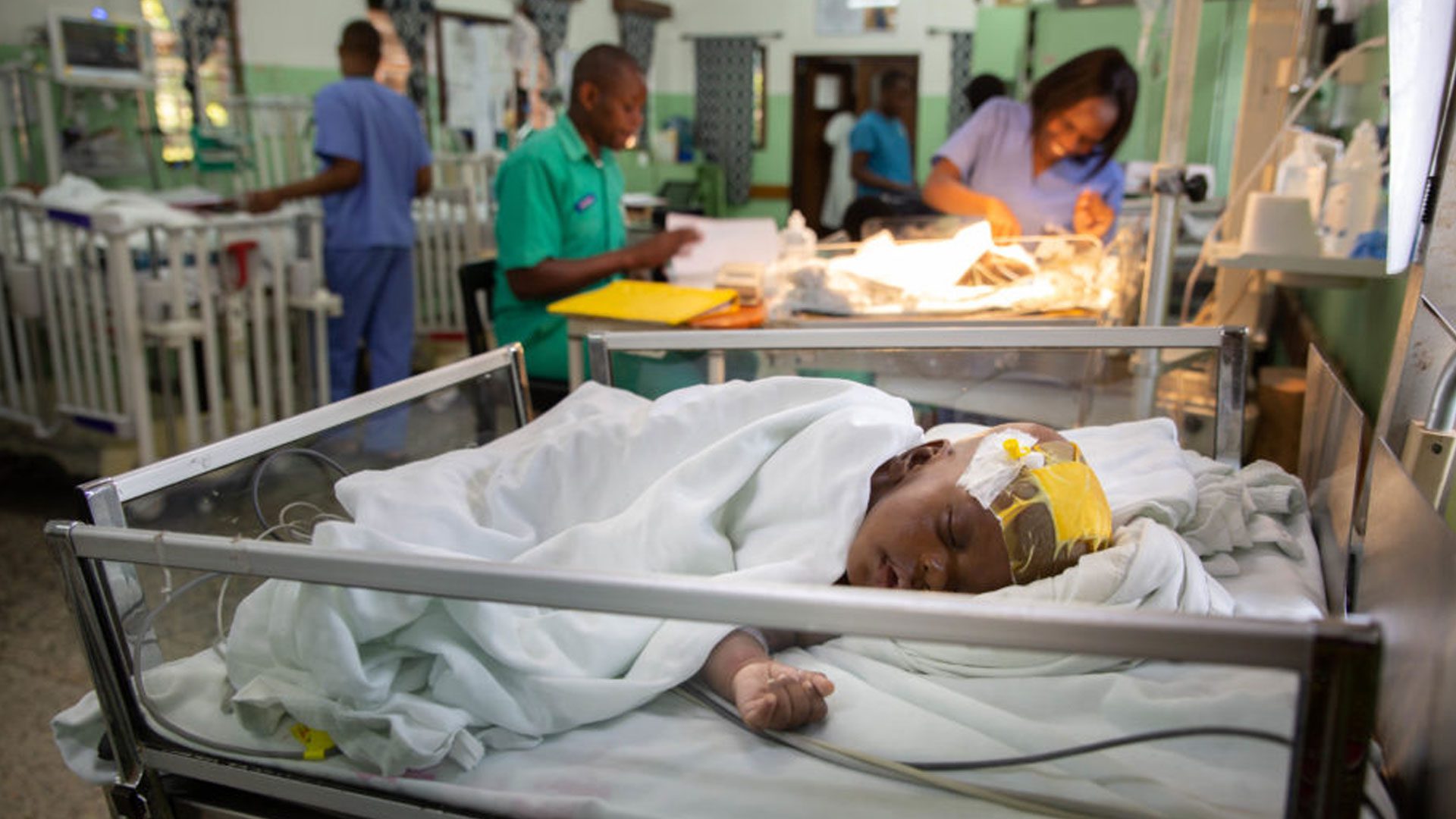
Object: Evidence from the CURE Children’s Hospital of Uganda (CCHU) suggests that treatment for hydrocephalus in infants can be effective and sustainable in a developing country. This model has not been broadly supported or implemented due in part to the absence of data on the economic burden of disease or any assessment of the cost and benefit of treatment. The authors used economic modeling to estimate the annual cost and benefit of treating hydrocephalus in infants at CCHU. These results were then extrapolated to the potential economic impact of treating all cases of hydrocephalus in infants in sub-Saharan Africa (SSA).
Methods: The authors conducted a retrospective review of all children initially treated for hydrocephalus at CCHU via endoscopic third ventriculostomy or shunt placement in 2005. A combination of data and explicit assumptions was used to determine the number of times each procedure was performed, the cost of performing each procedure, the number of disability-adjusted life years (DALYs) averted with neurosurgical intervention, and the economic benefit of the treatment. For CCHU and SSA, the cost per DALY averted and the benefit-cost ratio of 1 year’s treatment of hydrocephalus in infants were determined.
Results: In 2005, 297 patients (median age 4 months) were treated at CCHU. The total cost of neurosurgical intervention was $350,410, and the cost per DALY averted ranged from $59 to $126. The CCHU’s economic benefit to Uganda was estimated to be between $3.1 million and $5.2 million using a human capital approach and $4.6 million–$188 million using a value of a statistical life (VSL) approach. The total economic benefit of treating the conservatively estimated 82,000 annual cases of hydrocephalus in infants in SSA ranged from $930 million to $1.6 billion using a human capital approach and $1.4 billion–$56 billion using a VSL approach. The minimum benefit-cost ratio of treating hydrocephalus in infants was estimated to be 7:1.
Conclusions: Untreated hydrocephalus in infants exacts an enormous price from SSA. The results of this study suggest that neurosurgical intervention has a cost/DALY averted comparable to other surgical interventions that have been evaluated, as well as a favorable benefit-cost ratio. The prevention and treatment of hydrocephalus in SSA should be recognized as a major public health priority.