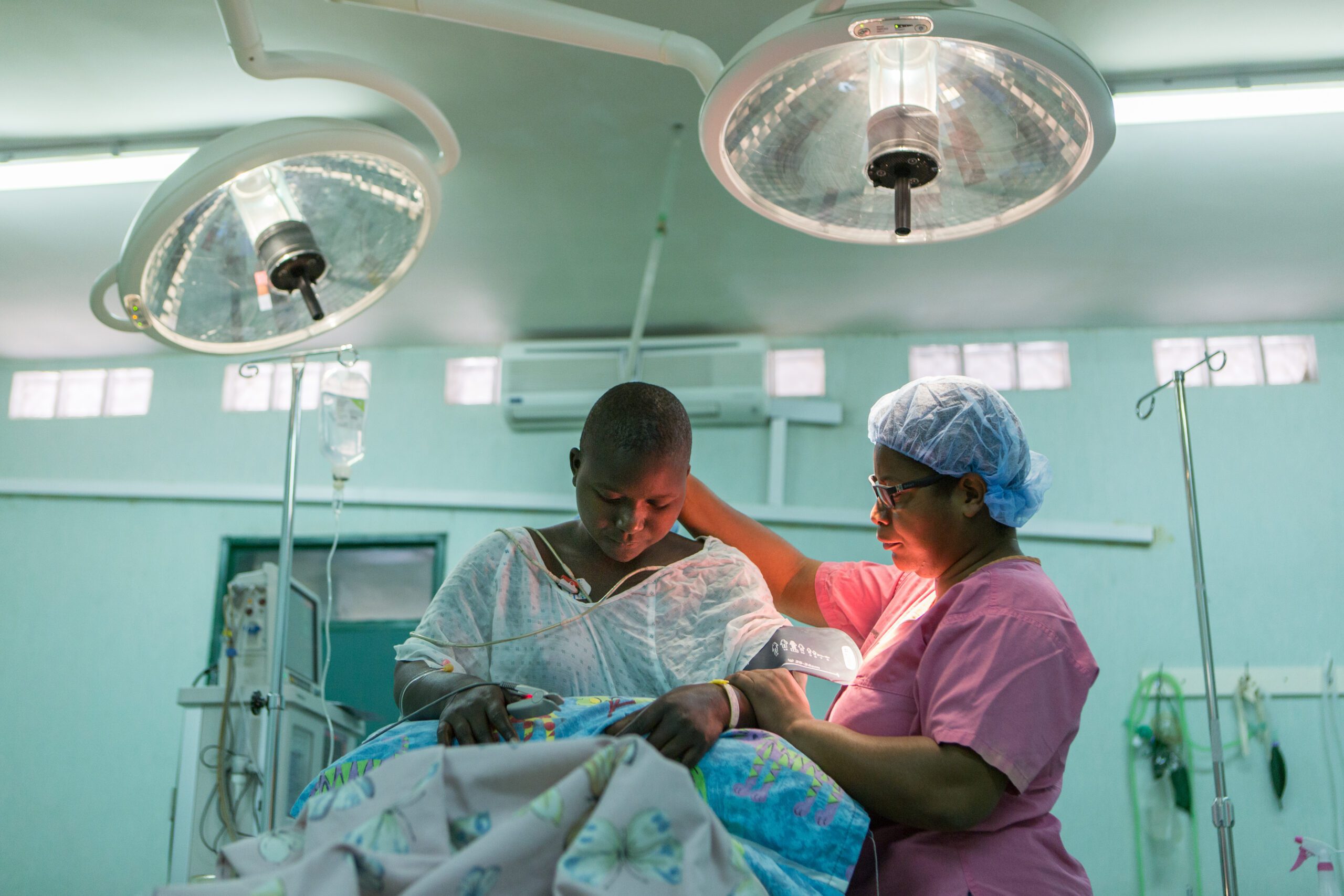
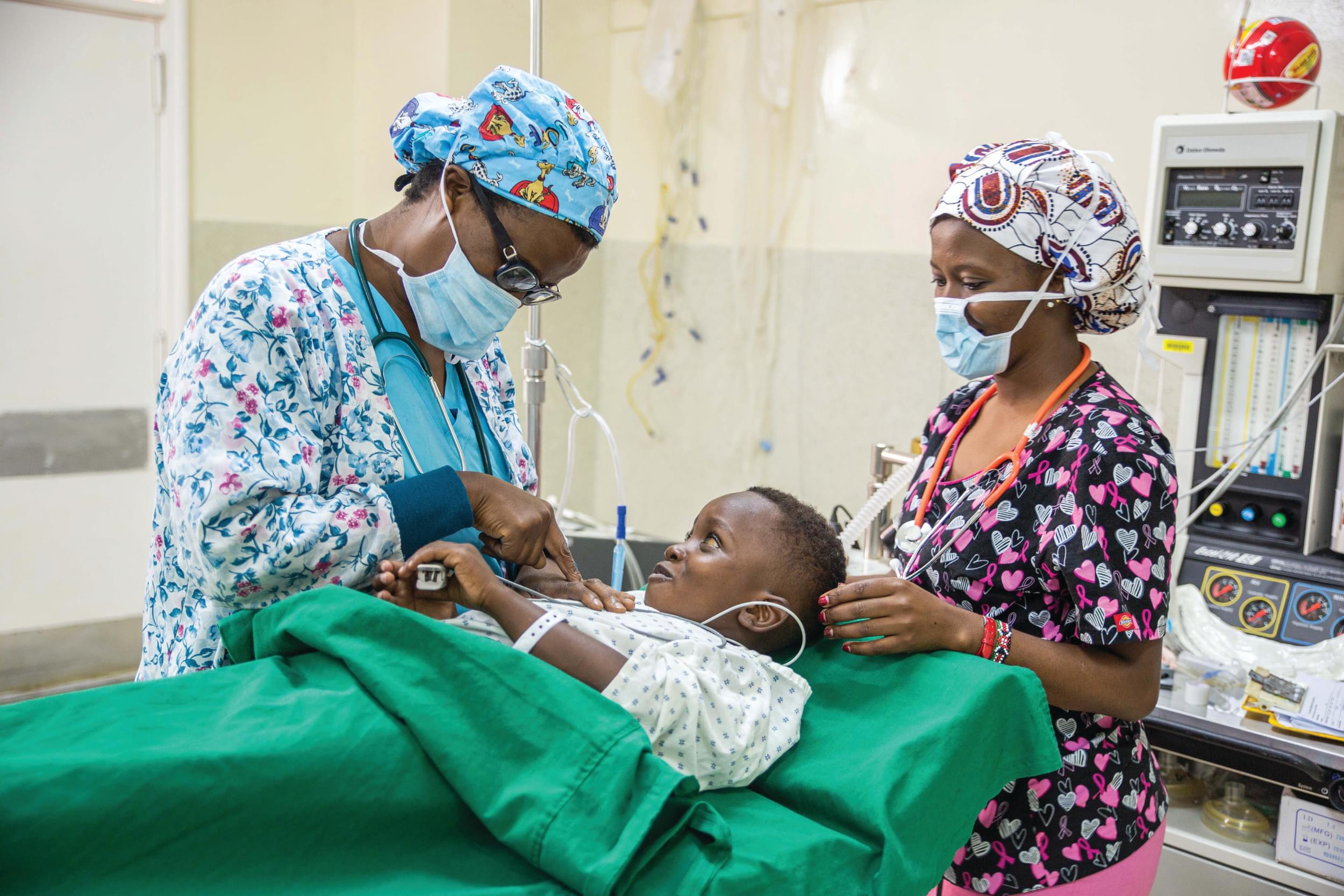
CURE International has pediatric surgical hospitals in seven low and middle-income countries, serving the population of those countries by providing essential musculoskeletal, neurosurgical, and plastic surgical care. Our non-governmental organization (NGO) plays a critical role in the healthcare of these countries through direct patient care, as well as Health System Strengthening (HSS) by training the next generation of surgeons, anesthetists, and nurses. In this article, we discuss our adaptation to the challenges faced by the COVID-19 pandemic, and how it further deepens the suffering of vulnerable children in desperate need of care.
No one is immune to the suffering caused by COVID-19 throughout the world. In Africa, where the majority of CURE’s hospitals are located, the effect of the pandemic was seen later than that in Europe and North America. As an organization, it has taken time and ongoing reflection to understand how our hospitals can best respond to this challenge.
In March, when the world looked on in concern and empathy for the enormous death toll in the Lombardy region in Italy and later in New York City, there seemed every likelihood that the countries where we serve in Africa would soon see similar suffering. Social overcrowding, limited access to running water, and packed public transport seemed fertile ground for the rapid spread of the virus. In addition to this, fragile healthcare systems with little surge capacity meant that there was every expectation we would see national healthcare collapse in the countries where we serve.
Given these expectations, our early preparations were to formulate a response to central questions such as: Could we (and should we) convert our operating rooms and anesthesia machines to create an Intensive Care Unit (ICU) to ventilate COVID-19 patients? What role should our hospitals play during the pandemic? Do we have the capability of caring for our co-workers if the government healthcare system becomes overwhelmed? Should we close our elective services, following the lead of hospitals all over the world?
We have the great privilege to be an integral part of the national healthcare services in the countries where we serve. We also have a responsibility to do our part during this particularly difficult time. We recognized that as specialist pediatric surgical hospitals, our area of expertise and our infrastructure was far removed from that needed to care for a critically ill COVID-19 patient. In the event that government hospitals became overwhelmed with patients needing respiratory support, we could be most effective in caring for children and adults with acute injuries who would otherwise further burden the government system. For now, it is a great blessing that this has not been required.

In the weeks that followed, elective surgical services were suspended globally, and we considered whether CURE should follow suit. Any cessation of elective surgical services can only be sensibly reversed after clear evidence that the escalation has peaked and a downward trend has occurred. Instead, we took each day at a time, following World Health Organization (WHO) guidelines with triage tents outside our hospitals, careful use of personal protective equipment (PPE) throughout our hospital, and additional precautions in the operating room (OR). Additionally, we moved to universal mask usage and donated cloth masks to all patients and their caregivers. Our service to children has continued throughout the pandemic to date, albeit with some necessary short interruptions as we have navigated issues such as regional quarantine and co-worker infection.
Through all the uncertainty, it has been a great encouragement to see the collaboration between our hospitals at this time. The leadership of our hospitals continues to meet frequently to share learning and challenges, as well as to discuss how best to share precious network resources. Locally, our hospitals have donated ventilators and PPE to the national response, and co-workers have supported local communities through the donation of supplies. We hope the goodwill and coordination this has fostered will continue for years to come.
As the virus escalation in the countries where we serve started to take hold, testing our patients for COVID-19 prior to surgical admission has been a significant focus. Our close collaboration with the government healthcare system, fostered over many years, has made testing possible in some of our hospitals, while private sector testing has been used at others. Testing is only one part of a hospital’s defense against the virus. We also have an ongoing dedication to the careful triage of patients and co-workers alike, robust PPE usage, and COVID-19 precautions in the Operating Room, which are central to keeping our patients, their families, and our team safe.
Our hospitals receive children with disabilities from all over the country where they serve. This national reach could be problematic during a pandemic where the capital city is often the primary hotspot for infection. Receiving patients and their caregivers from rural areas, where COVID-19 has yet to take hold, carries the risk that they could return with the condition and be a vector of spread. To mitigate this, many of our hospitals took the early step of limiting their referral base to the local environs. In other countries, there was an enforced travel restriction, sometimes lasting for several months, having the same effect.
Where to go from here?
This leads us to the long-term effect of the pandemic on the well-being of the children whom we serve. At the time of writing this, in most of the countries where CURE operates, we are starting to see evidence of being past the peak of the first wave of infection.
There is now a greater awareness that COVID-19 will be with us for longer than was originally anticipated. Elective services globally have restarted despite ongoing high positivity rates and while confronting second waves of the pandemic.
Our surgical services have continued, but there has been an inevitable drop in surgeries performed due to COVID-19 precautions, regional mandatory quarantine, and managing local COVID-19 exposure. For example, our hospital in Ethiopia has several thousand children waiting to access care. This pandemic has resulted in an even longer wait for essential treatment for some of the most vulnerable children in the world.
To help mitigate the wait for specialized surgical services, CURE and our partners continue to invest in training the next generation of surgeons. Our focus is to provide clinical excellence while training local surgeons to do the same. These highly capable surgeons are leading their own training programs, and in time, children will be able to access timely, local, and excellent care. However, all of these efforts are being severely compromised by the far-reaching effects of this pandemic. To continue this necessary training, targeted investment in infrastructure and training is urgently needed.
CURE’s work and that of our partners who strive to transform the lives of children and their communities are dependent upon the generosity of thousands of people who share our vision and are part of this journey. We invite others to join us so that the valuable ground gained is not lost and greater national resilience is achieved to combat the effects of this pandemic and beyond.
About CURE International
CURE International is a Christian nonprofit organization that operates a global network of pediatric surgical hospitals, which serve one of the world’s most marginalized and vulnerable populations – children with disabilities. Patients at CURE hospitals suffer from orthopedic, neurosurgical, and maxillofacial conditions that limit their mobility/functionality and opportunities for education and employment. In addition to world-class clinical service, CURE intentionally ministers to the emotional and spiritual needs of patients in its care and invests in training programs that aim to equip the next generation of health workers and strengthen national health care systems. Since inception, CURE has conducted more than 5.3 million patient visits and 330,000 surgical procedures around the world. For more information, visit https://cure.org/.