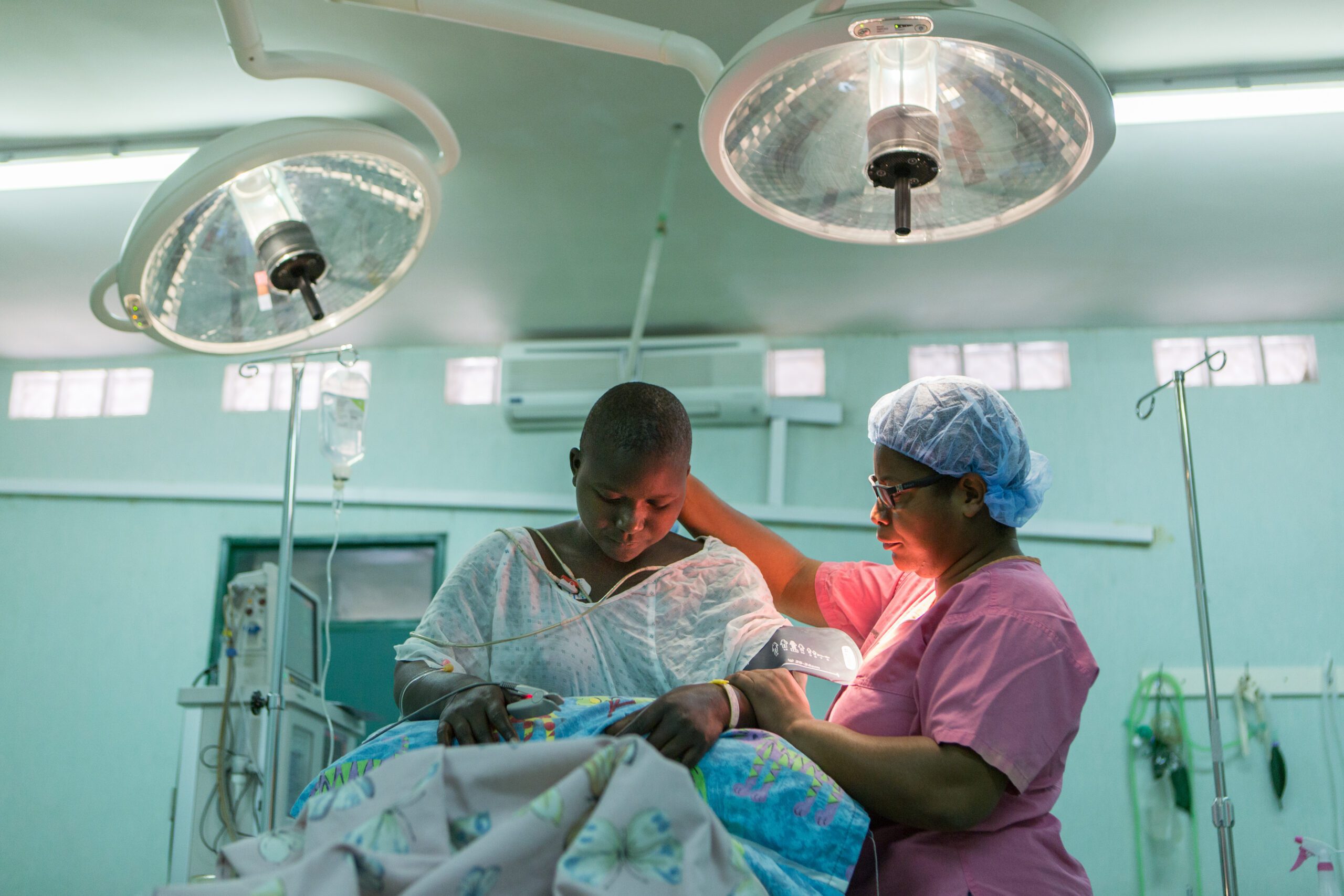
When we use the term “safe surgery,” we don’t mean just the fact that the surgery is being performed by a skilled, experienced surgeon. This term encapsulates the entire surgical system—is it considered “safe” from start to finish, from admitting a patient all the way through to their discharge? One of the key findings of the 2015 Lancet Commission on Global Surgery was that: “5 billion people do not have access to safe, affordable surgical and anaesthesia care when needed. Access is worst in low-income and lower-middle-income countries, where nine of ten people cannot access basic surgical care.”
It can be hard to picture 5 billion people. After all, that’s the majority of the world’s population. But at CURE Uganda, it’s easy to picture one little baby—one baby that has been born with a myelomeningocele or developed an infection that has led to hydrocephalus. What does “safe, affordable surgical and anesthesia care” look like here?

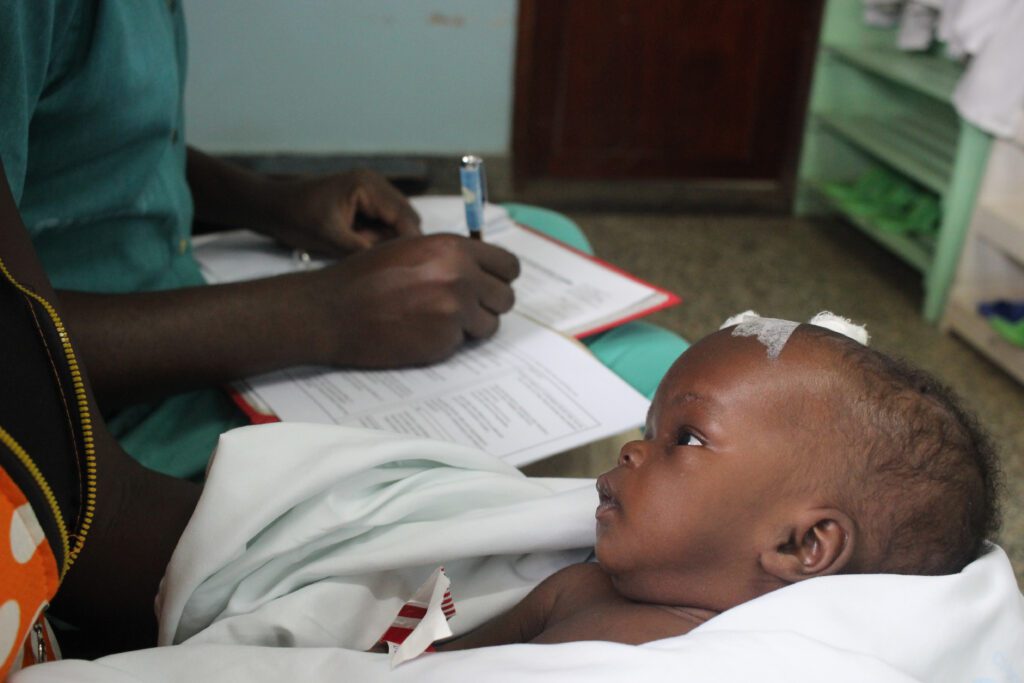
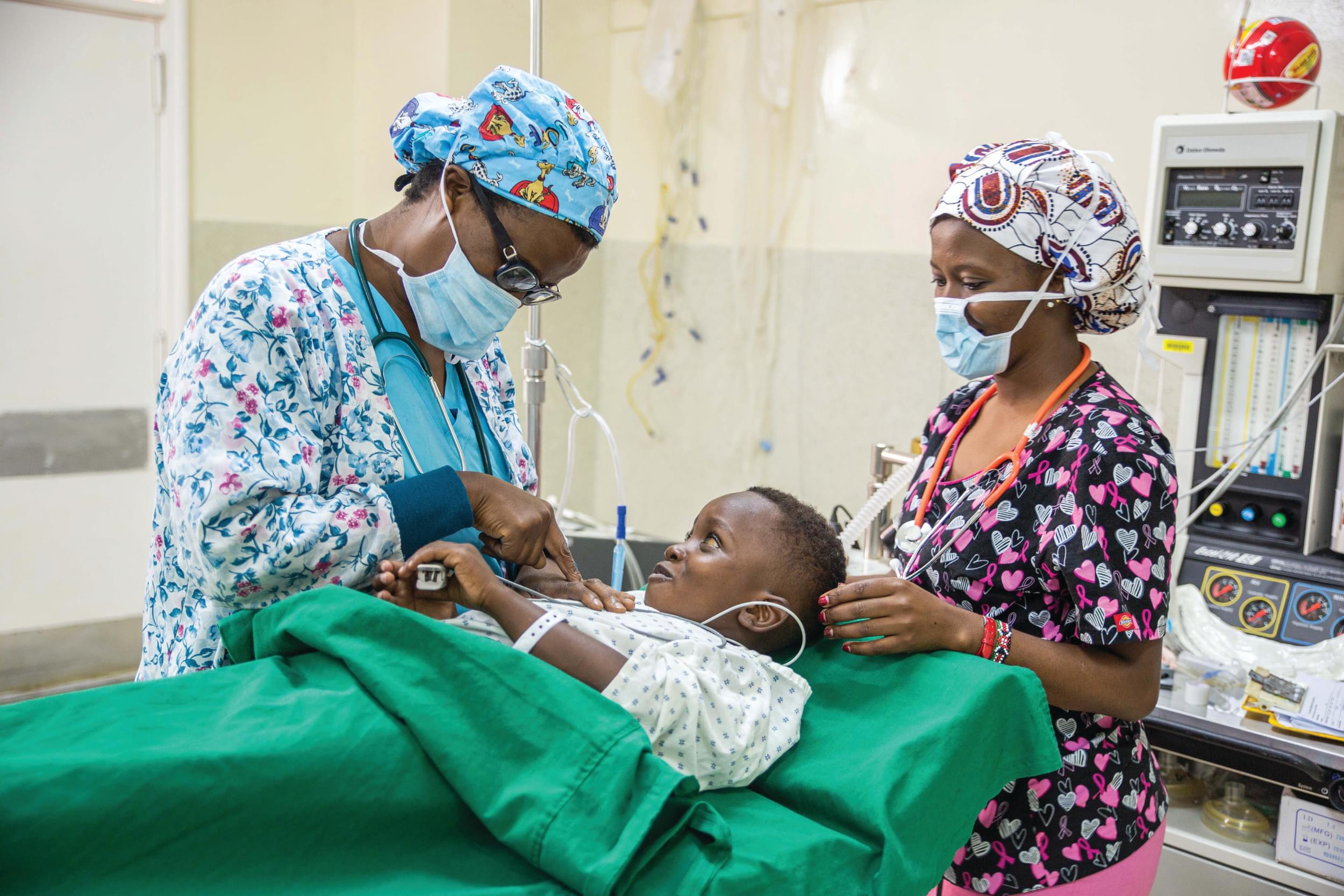
For CURE Uganda safe surgery at our neurosurgical specialty hospital includes a number of different locations, systems, and teams, ranging from the nurses who fill out the WHO Safe Surgery Checklist, to the procurement team that ensures we have the sutures, medicines and materials we need, to the PACU and ICU teams who ensure our smallest patients recover from surgery well. Each of these teams and subsystems have to be working effectively and communicating clearly within their team and with other teams or the entire process would fall apart—with catastrophic results for our patients. Thankfully, each member of the CURE staff is highly trained, and due to the generosity of donors and this incredible staff, we are able to provide world-class surgical services in an LMIC (low- or middle-income country).
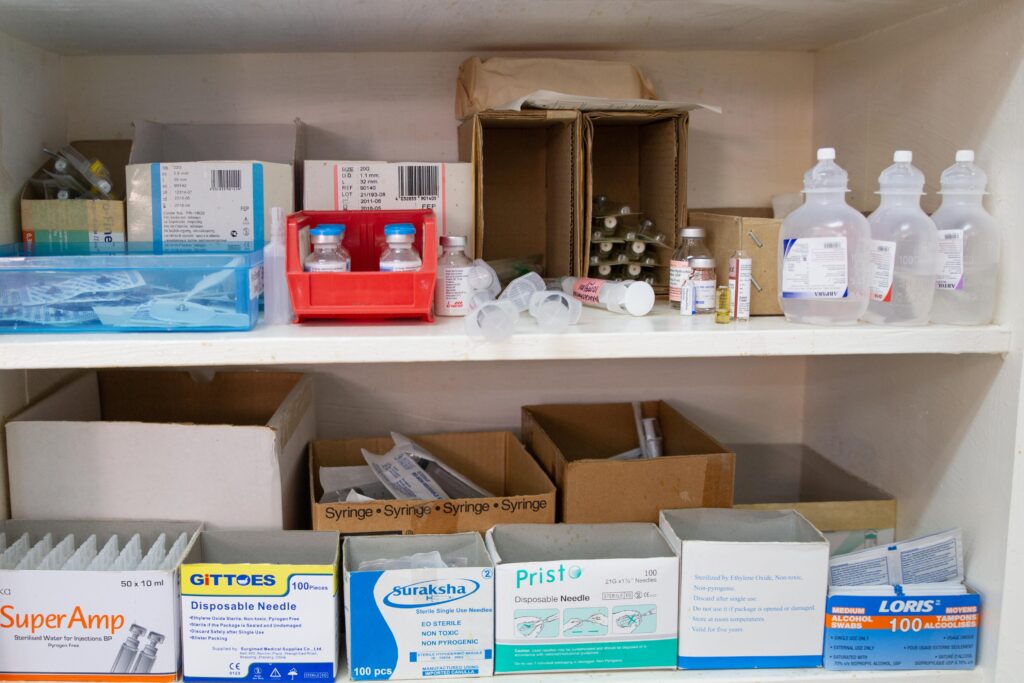

While some of these systems, like working lights and power, may seem like a given, in the small city of Mbale and in many other places in Uganda, reliable electricity cannot be taken for granted. CURE Uganda has a generator and an entire team of maintenance workers who ensure that we have the electricity we need, and that the power doesn’t go out halfway through an operation. Additionally, we work closely with our partner, International Aid, to be sure all our equipment is in working order, including cautery and suction machines, flexible endoscopes, and anesthesia and monitoring equipment.


CURE Uganda’s procurement team ensures that we have the right materials and equipment for surgery when we need them. This stands in stark contrast to many local hospitals in LMICs, where patients are often required to gather and purchase medicines and supplies, including blood, before medication can be given or surgery performed. Having ready access to all the sutures, anesthesia, medications, and dressings needed is cited by our nursing and anesthesia teams as one of the reasons they so enjoy working at CURE Uganda.
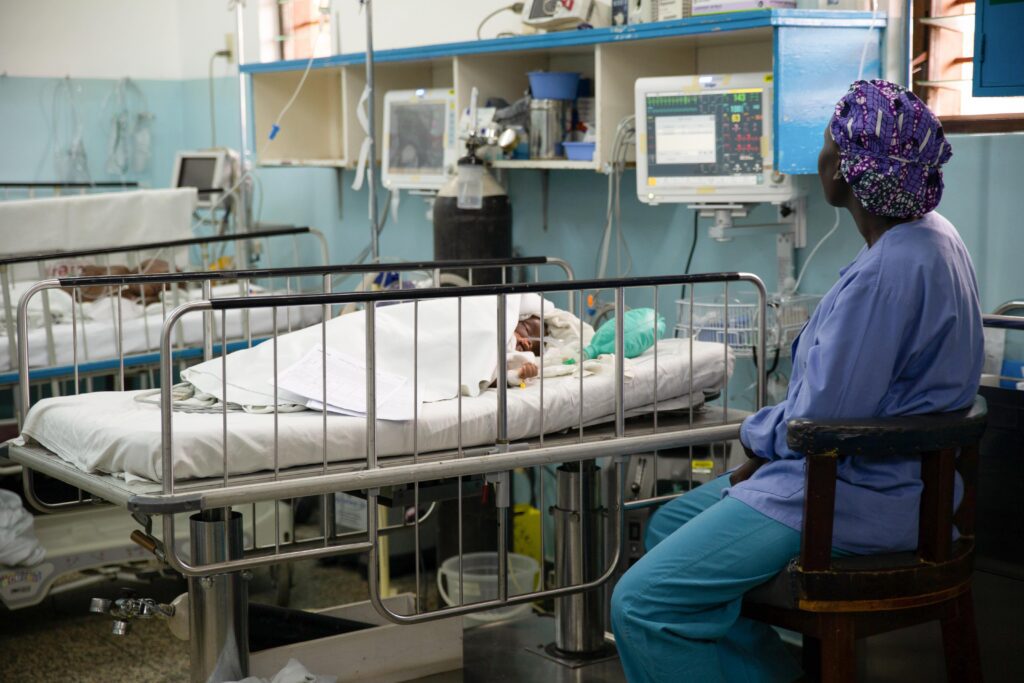
Caring for patients pre- and post-surgery is another piece of the system that often can be overlooked but is absolutely essential, as the World Bank’s Essential Surgery volume of Disease Control Priorities identifies: “The surgical capabilities required are not only those related to performing operations. Surgical care also involves preoperative assessment, including the decision to operate; provision of safe anesthesia; and postoperative care.(1)” CURE Uganda is able to provide care at each of these points, with our laboratory, X-ray, CT scanner, ultrasound, post-operative care unit (PACU), and intensive care unit (ICU). Our anesthetist team, led by Dr. Fred Musana and Dr. Fred Bulambu, monitors each patient from start to finish, and the entire OR team uses the WHO Safe Surgery Checklist for every patient.

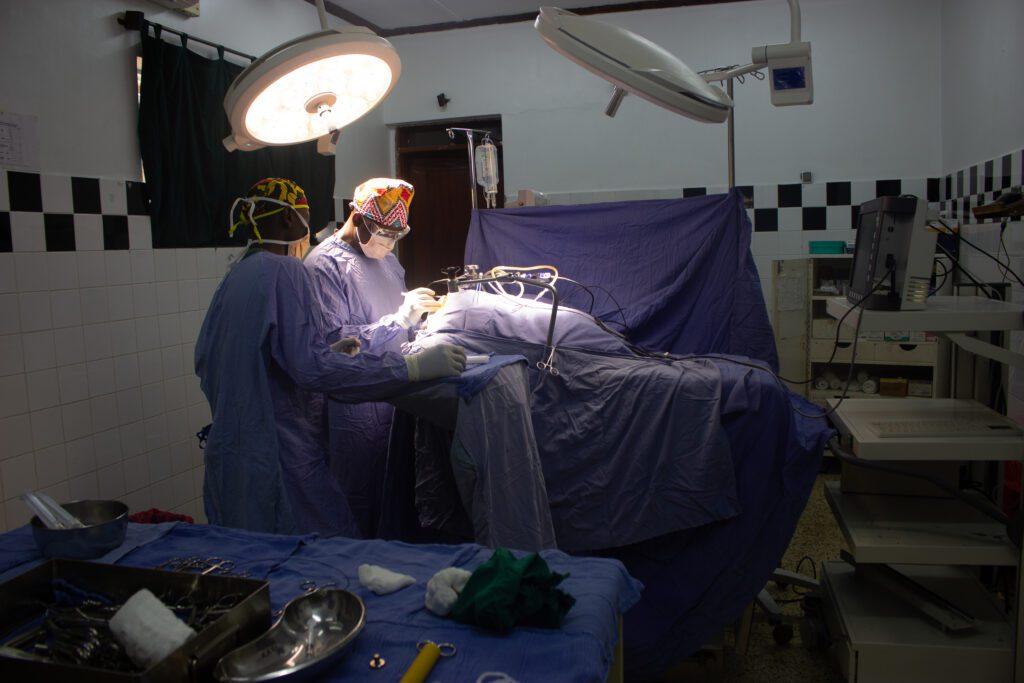
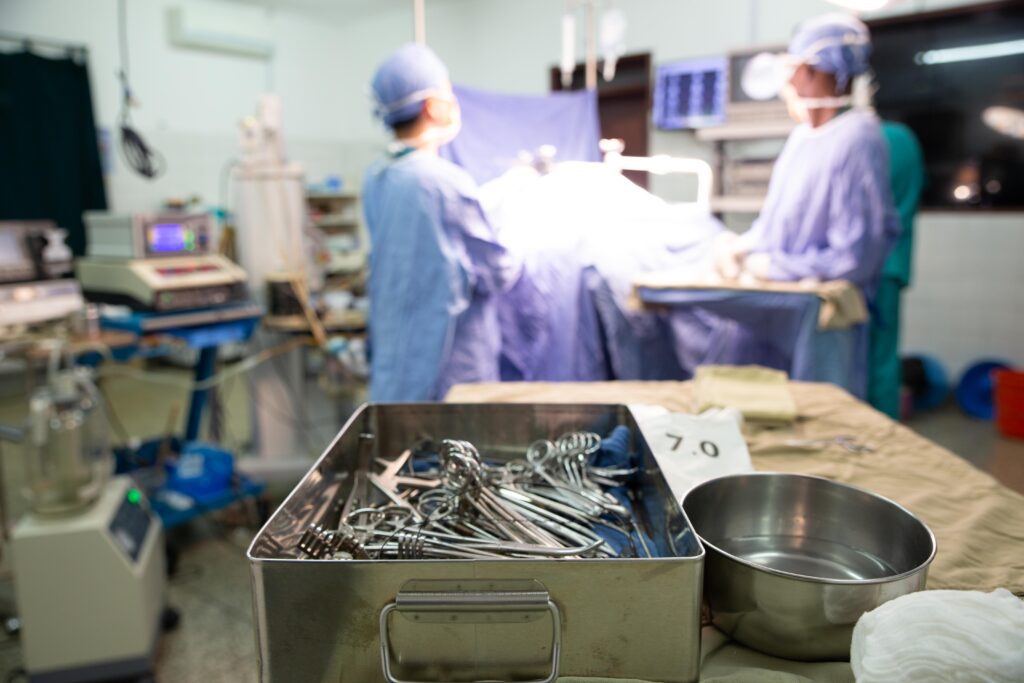
Of course, none of these systems would be effective if our neurosurgeons were operating with contaminated equipment. Sterile Processing Educational Charitable Trust (SPECT) is one of the only charities worldwide dedicated to training healthcare workers in LMICs on sterile processing practices. According to SPECT, properly sterilized surgical instruments lead to reduced infection rates, improved healing and better overall patient outcomes. However, many hospitals in LMICs lack equipment, training, and understanding of sterile processing standards and infection control procedures(2). At CURE Uganda, we recognize the vital importance of sterile processing and take it very seriously. Our sterile processing team, some of whom have been serving at CURE Uganda since it first started 19 years ago, use the sluice room and autoclaves connected to the OR with best practices for sterilizing surgical instruments. This essential team ensures that each piece of equipment is not just clean but sterile and prepared for the neurosurgeons and OR team.


Zooming out beyond the lab, OR, PACU, and ICU, there is another lens through which we can view the safe surgery system and the necessary components. In a talk to Mercy Ships last year, Dr. Mark Shrime, director of the Center for Global Surgery Evaluation, identified four key pillars of safe surgery: Availability, Safety, Affordability, and Timeliness. Safety has already been discussed above, and CURE Uganda also tackles each of these other three pillars in a number of different ways.
Availability
At CURE, we welcome any patient with a neurosurgical condition that comes through our gate. While the majority of our patients are infants with spina bifida and hydrocephalus, we also treat children and adults with brain tumors, traumatic brain injuries, and other neurosurgical issues. Patients are often referred here from other health centers and hospitals and come from neighboring countries such as Kenya and South Sudan.
While we try to get the word out about our services by TV, radio, social media, and word of mouth, we recognize that we are most likely only seeing about 20-30% of the hydrocephalus cases in Uganda, and about 20-30% of the cases of spina bifida. Based on CURE’s experience, actual surgical volumes, and using conservative prevalence rates from the National Institutes of Health, CURE Uganda estimates that 3,600 – 5,400 children in Uganda are born with or acquire hydrocephalus each year, and about 600-800 children per year are born with spina bifida. While we’d love to provide surgery for each one of these children, that would require a massive scale-up of our facilities, which are already full to bursting. During the previous fiscal year CURE Uganda provided surgery to 1,530 patients, which is a 15.6% increase from the year before! We frequently have a full ward, full overflow hostel, and resort to having patients sleeping on mattresses on the floor due to lack of bed space. We do have plans underway to expand our ward and ICU and are looking forward to being able to serve more children as those projects are completed, but the need remains great.

In order to increase availability to CURE’s services, we host mobile clinics in five other cities: Gulu, Lira, Jinja, Kampala, and Mbarara. Our doctors, clinical officers, spiritual team, and physical therapist travel to those mobile clinics and faithfully provide review services there. Because traveling to Mbale for follow-up appointments can be challenging and expensive for patients and their caregivers, this allows us to go to them, and allows more patients to receive the follow-up care that they need.
Affordability
While each neurosurgery on average costs roughly $1,500.00 USD, patients’ families are only asked to make a contribution of UGX 950,000 (approximately $260.00 USD) toward this total cost of care. The rest of the cost is covered by charitable contributions from CURE International’s sponsors, which we are so grateful for. However, many people in Uganda, especially in rural areas, make less than $100.00 a month, so this can still be a significant hurdle and stressor. Thankfully, CURE Uganda has a wonderful team of social workers, who carefully take the time to work with each family and assess their level of need. No child is turned away for lack of the family’s finances to contribute towards the cost of care. Families are encouraged to contribute to their child’s bill through payment plan options as they come back for each review appointment. In many cases of severe need, even the local family contribution requested can be covered by additional local donations. CURE Uganda is working tirelessly to ensure every child with the urgent medical conditions we treat has access to the highest quality surgical care.
Recently, we launched the CURE Chicken Project, which provides parents who attend three consecutive review appointments with a young hen and rooster, so they can begin their own small income-generating project, selling eggs, chicks, or both!
Timeliness
Roads in Uganda have improved in recent years, thanks to government projects and Chinese investments, but it still can be a challenge for patients to come to Mbale, the small town where CURE Uganda is located. Thankfully, the bus stop is within walking distance of the hospital, and patients are welcomed 24/7, with doctors and nurses on call.

Children with spina bifida usually come to CURE quickly, often a day or two after they are born, since their condition is more immediately obvious. For parents with a child with post-infectious hydrocephalus, their stories can be more complicated. Depending on a patient’s location, it may take several months for them to notice their baby’s head is increasing in size, then visit their local health clinic, then be referred on to a larger hospital, and then referred to us. Unfortunately, the infection can continue to ravage their child’s brain during this time. We are known by many referral hospitals in many cities throughout Uganda, who frequently refer patients to us. Additionally, we have a CURE Neuro partnership with a CURE-trained neurosurgeon and care coordinator in Mbarara, out in Western Uganda.
We’re continuing to work on getting the word out about CURE Uganda and the services we provide, and as mentioned above, last year our number of surgeries provided increased by more than 15%. We are thankful for God’s grace in sending us more patients, and the stamina of our surgeons, doctors, nurses, and social workers who are handling this increased patient load with great faithfulness.
From a systems perspective, the level of safe, affordable surgical and anesthetic care that CURE Uganda is able to provide is astonishing. Each team member and subsystem works together to provide world-class care to children who desperately need neurosurgical treatment. We are thankful for each person working at CURE who gives their best each day to make our safe surgery system work effectively to save and transform lives.
- Mock, C. N., Donkor, P., Gawande, A., Jamison, D. T., Kruk, M. , et. al. 2015. “Essential Surgery: Key Messages of this Volume”. In: Disease Control Priorities (third edition): Volume 1, Essential Surgery, edited by H. Debas, P. Donkor, A. Gawande, D. T. Jamison, M. Kruk, C. N. Mock. Washington, DC: World Bank. Page 2.
- SPECT Overview. Christina Fast and Dr. Olive Fast. August 27, 2019.
About CURE International
CURE International is a Christian nonprofit organization that operates a global network of pediatric surgical hospitals, which serve one of the world’s most marginalized and vulnerable populations – children with disabilities. Patients at CURE hospitals suffer from orthopedic, neurosurgical, and maxillofacial conditions that limit their mobility/functionality and opportunities for education and employment. In addition to world-class clinical service, CURE intentionally ministers to the emotional and spiritual needs of patients in its care and invests in training programs that aim to equip the next generation of health workers and strengthen national health care systems. Since inception, CURE has conducted more than 5.3 million patient visits and 330,000 surgical procedures around the world. For more information, visit https://cure.org/.