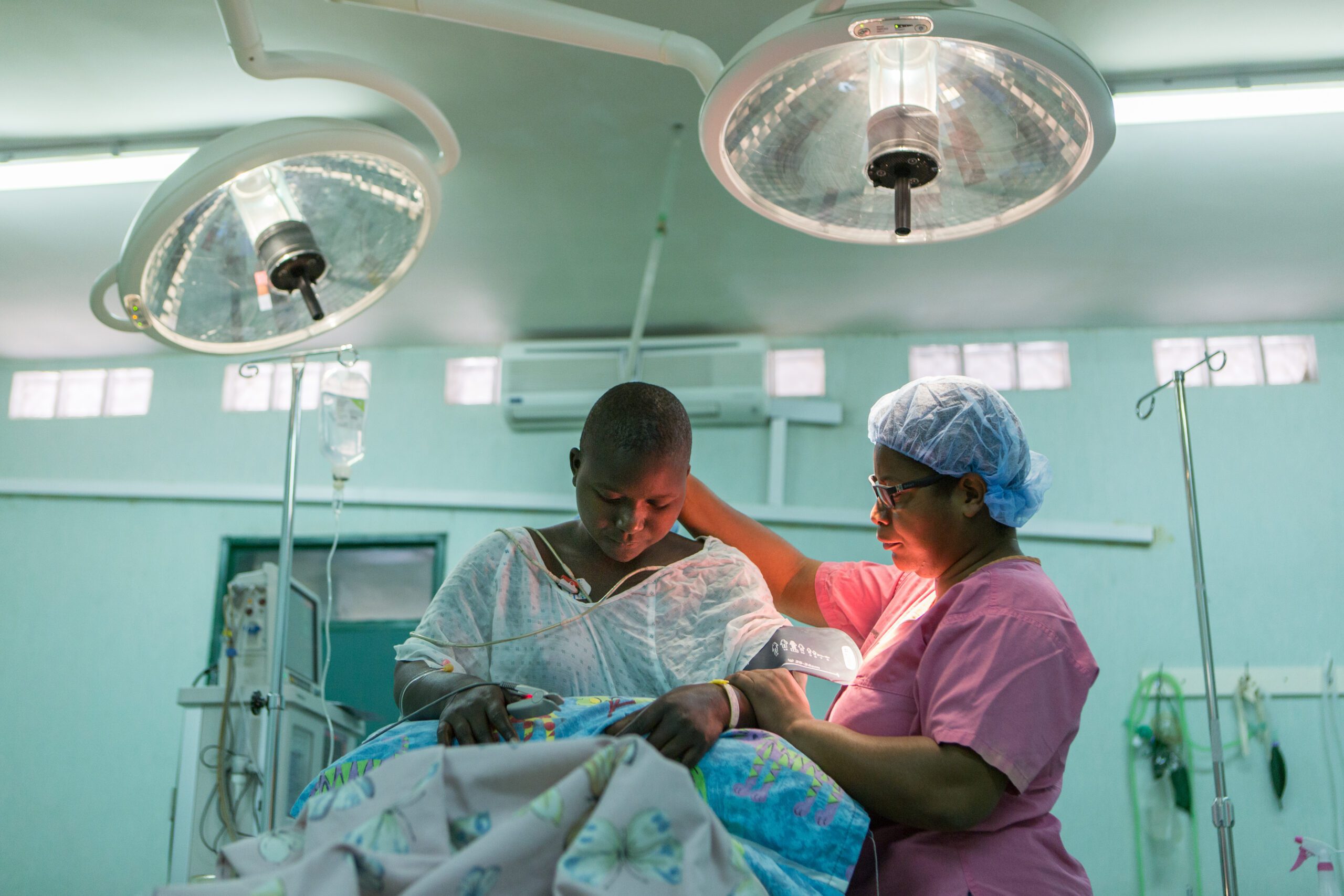
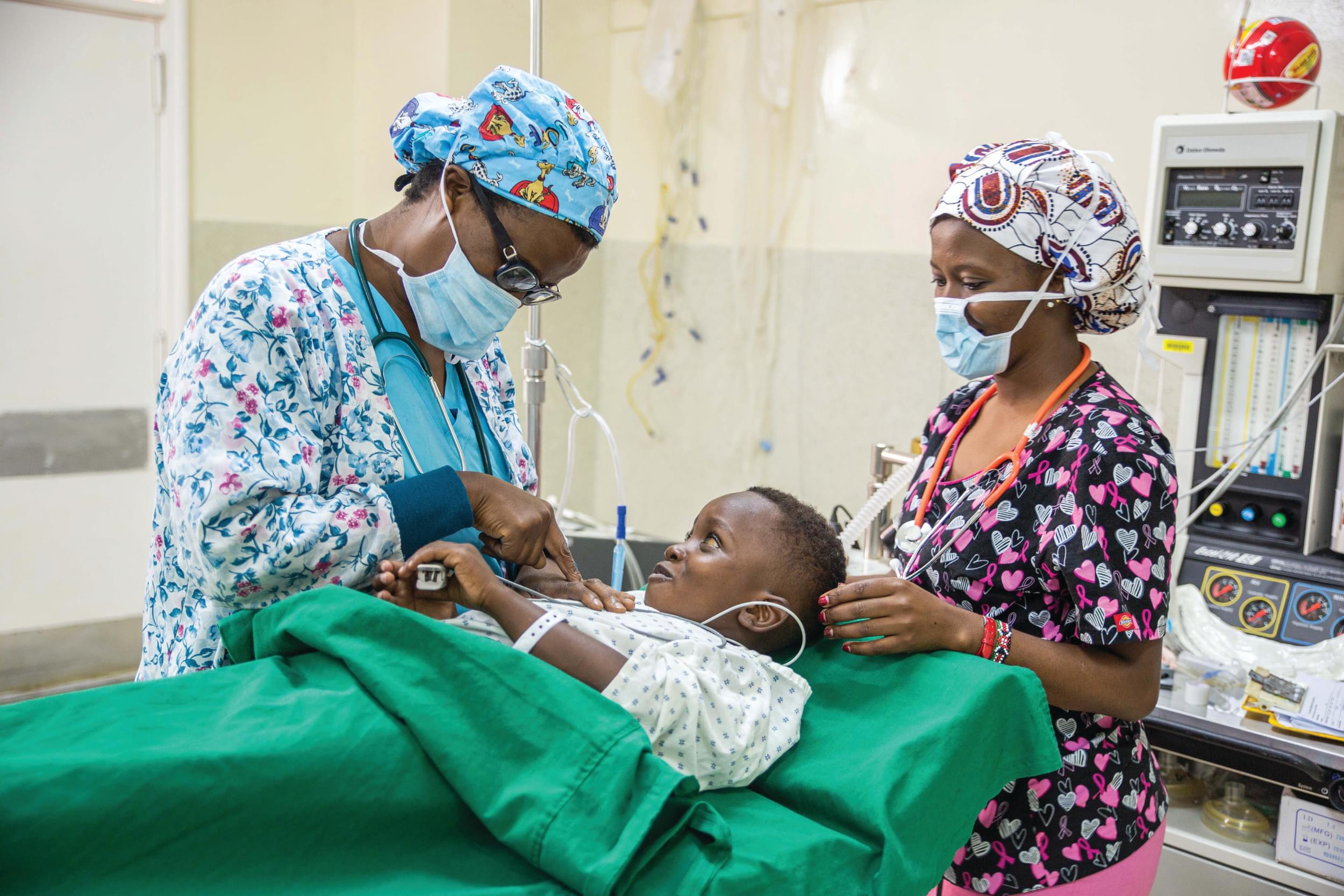
Have you ever wondered what happens when a child goes in for neurosurgery? In this piece, Dr. Micheal Ogwal, the former Medical Officer at CURE Uganda, walks us through the surgery experience.
Surgery can be an intimidating thing to many, and the thought of brain surgery on a child doesn’t make things any better for an anxious caregiver. Endless questions about the child’s safety form the bulk of the conversation in taking consent the day before surgery.

The arrival at the OR waiting area may be even more intense. The beeping machines at the Post Anesthesia Care Unit (PACU), the red line, and the masked nurses, surgeons, and anesthetist welcome a starving baby and an anxious caregiver accompanied by the ward nurse.
The OR nurses have mastered the art of comforting the babies and the caregivers. This is ably done alongside ensuring patient safety. They double check with the ward nurse and caregiver to ensure the prescribed NPO was maintained along with the vital signs trends.

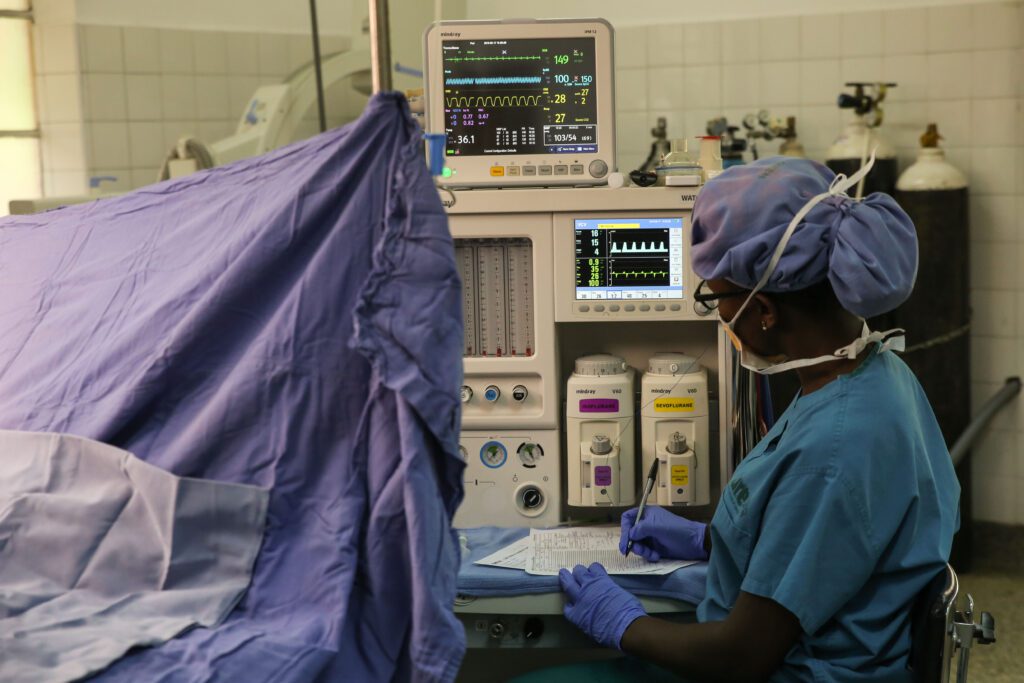
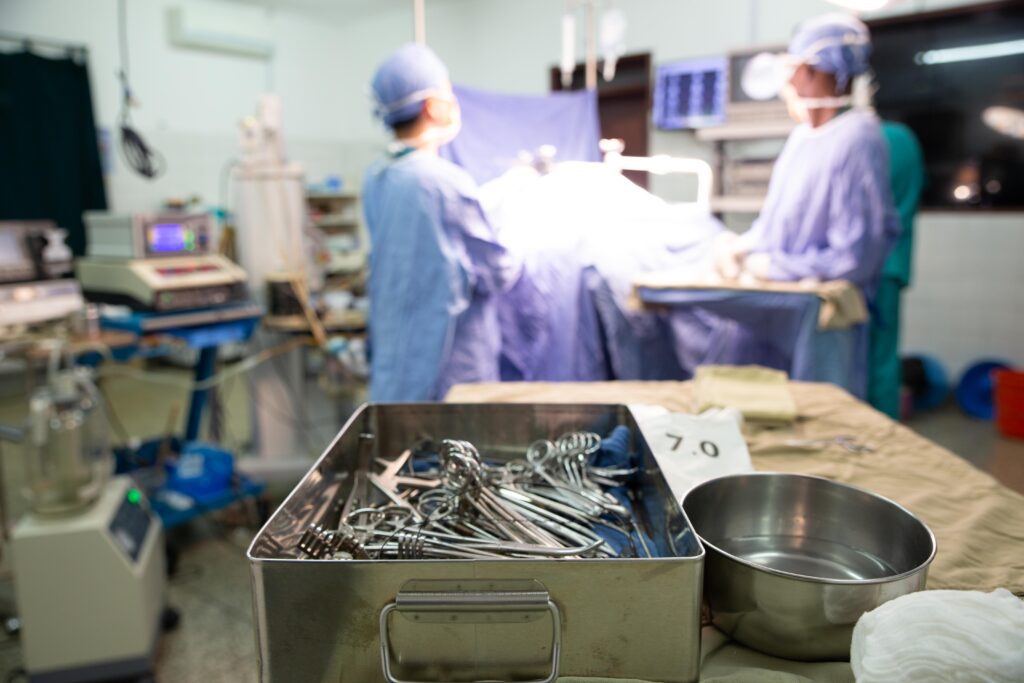
The swaddled baby in an OR grown is carried in the warm hands of an anesthetist who will ensure the baby sleeps calmly through the surgery. The running nurse, on the other hand, confirms presence and functioning of the equipment required for the proposed surgery. She will confirm the sterility of the equipment as well. The scrub nurse donned in a gown arranges the surgical instruments.
The surgeon who “captains the ship” positions the patient for surgery before the surgical checklist is done and proceeds to mark the surgical site.
A prayer is said and the incision made. The surgery proceeds, each member of the team aware of their specific roles and complementing each other, very much like the image of the body of Christ described in 1 Corinthians 12.

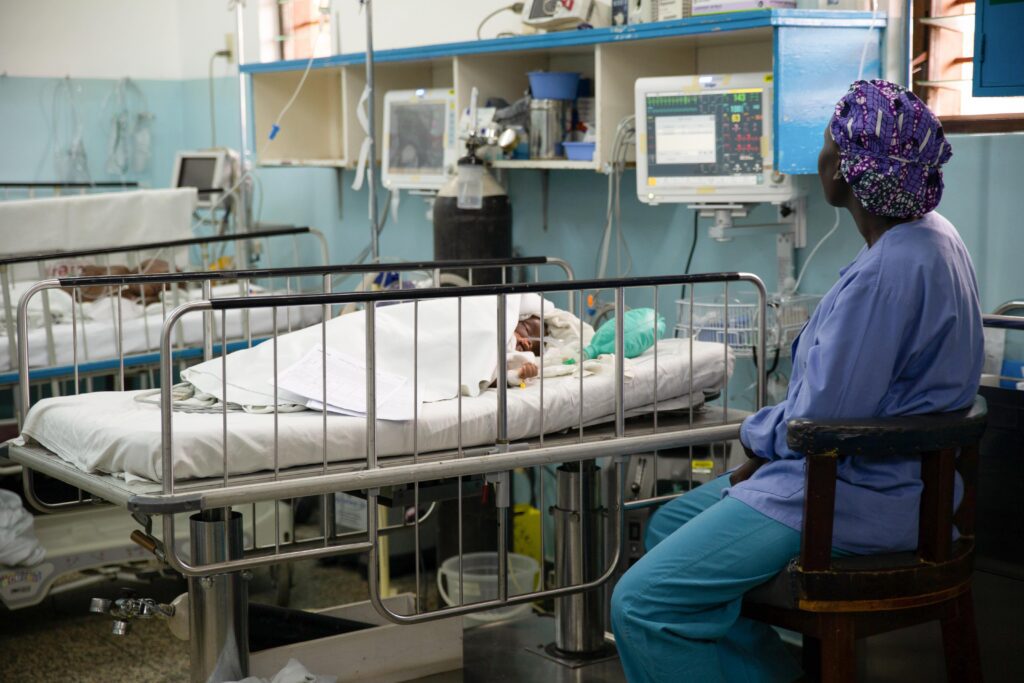
The PACU team ensures complete recovery of the patient before transit to the ICU, where the patient will continue to be monitored and will be reunited with their caregiver. The healing process has begun.
About CURE International
CURE International is a Christian nonprofit organization that operates a global network of pediatric surgical hospitals, which serve one of the world’s most marginalized and vulnerable populations – children with disabilities. Patients at CURE hospitals suffer from orthopedic, neurosurgical, and maxillofacial conditions that limit their mobility/functionality and opportunities for education and employment. In addition to world-class clinical service, CURE intentionally ministers to the emotional and spiritual needs of patients in its care and invests in training programs that aim to equip the next generation of health workers and strengthen national health care systems. Since inception, CURE has conducted more than 5.3 million patient visits and 330,000 surgical procedures around the world. For more information, visit https://cure.org/.